Posted on October 13, 2017 I Written By Janae Sharp
Healthcare as a Human Right. Physician Suicide Loss Survivor. Janae writes about Artificial Intelligence, Virtual Reality, Data Analytics, Engagement and Investing in Healthcare. twitter: @coherencemed
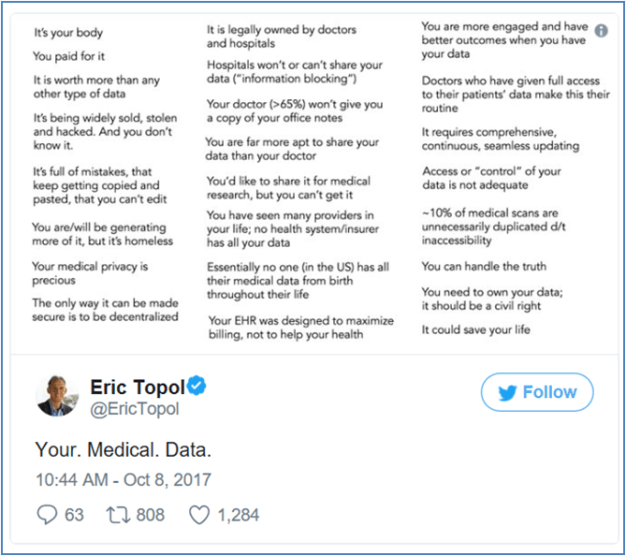
Health record interoperability and patient data is a debated topic in Health IT. Government requirements and business interests create a complex exchange about who should own data and how it should be used and who should profit from patient data. Many find themselves asking what the next steps in innovation are. Patient data, when it is available, is usually not in a format that is visible and useful for patients or providers. The debate about data can distract from progress in making patient data visible and useful.
Improvements in HealthIT will improve outcomes through better data interpretation and visibility. Increasing the utility of health data is a needed step. Visibility of patient data has been a topic of debate since the creation of electronic health records. This was highlighted in a recent exchange between former vice president Joe Biden and Judy Faulkner, CEO of Epic Systems.
Earlier this year at the Cancer Moonshoot, Faulkner expressed her skepticism about the usefulness of allowing patients access to their medical records. Biden replied, asking Faulkner for his personal health data.
Faulkner was quick to retort, questioning why Mr. Biden wanted his records, and reportedly responded “Why do you want your medical records?” There are a thousand pages of which you understand 10.”
My interpretation of her response-“You don’t even know what you are asking. Do not get distracted by the shiny vendor trying to make money from interpreting my company’s data”
As reported in Politico Biden–and really, I think that man can do no wrong, responded, “None of your business.”
In the wake of the Biden Faulkner exchange, the entire internet constituency of Health IT and patient records had an ischemic attack. Since this exchange we’ve gone on to look at interoperability in times of crisis. We’ve had records from Houston and Puerto Rico and natural disasters. The importance of sharing data and the scope of useful data is the same.
During what I call the beginning of several months of research about the state of interoperability I started reading about the Biden and Faulkner exchange. This was not the first time I had been reading extensively about patient data and if EHR and EMR data is useful. It just reminded me of the frustrations I’ve heard for years about EHR records being useless. Like many of us, I disappeared down the rabbit hole of tweets about electronic health records for a full day. Patient advocates STILL frustrated by the lack of cooperation between EHR and EMR vendors found renewed vigor; they cited valid data. Studies were boldly thrown back and the exchange included some seriously questionable math and a medium level of personal attack.
Everyone was like, Are we STILL on this problem where very little happens and it’s incredibly complex? How? How do we still not have a system that makes patient data more useful? Others were like, Obviously it doesn’t make sense because A) usefulness in care, and B) money.
Some argued that patients just want to get better. Others pointed out that acting like patients were stupid children not only causes a culture of contempt for providers and vendors alike, but also kills patients. Interestingly, Christina Farr CNBC reported that the original exchange may have been more civil than originally interpreted.
My personal opinion: Biden obviously knew we needed to talk about patient rights, open data, and interoperability more. It has had more coverage since then. I don’t know Faulkner, but it sounds like a lot of people on Twitter don’t feel like she is very cooperative. She sounds like a slightly savage businesswoman, which for me is usually a positive thing. I met Peter from Epic who works with interoperability and population health and genomics and he was delightful.
Undeniably, there is some validity to Judy’s assertion that the data would not be useful to Biden; EHR and EMR data, at least in the format available from the rare cooperative vendors, is not very useful. They are a digital electronic paper record. I am willing to bet Biden–much as I adore the guy–didn’t even offer a jump drive on which to store his data. The potential of EHR data visualization to improve patient outcomes needs more coverage. Let’s not focus on the business motivations of parties that don’t want to share their data, let’s look at potential improvements in data usefulness.
It was magic because I had just had a conversation about data innovation with Dr. Michael Rothman. An early veteran in the artificial intelligence field, Dr. Rothman worked in data modeling before the AI winter of the 80s and the current resurgence in investment and popularity. He predates the current buzz cycle of blockchain and artificial intelligence everything. With many data scientists frustrated by an abandonment of elegant, simple solutions in favor of venture capital and sexy advertising vaporware, it is timely to look at tools that improve outcomes.
In speaking with Dr. Rothman, I was surprised by the cadence of his voice, he asked me what I knew about the history of artificial intelligence, and I asked him to tell his data story. He started by outlining the theory of statistical modeling and data dump in neural net modeling. His company, PeraHealth, represents part of the solution for making EMR and EHR data useful to clinicians and patients.
The idea that data is going to give you the solution is, in a sense, slightly possible but extremely unlikely. If you look at situations where people have been successful, there is a lot of human ingenuity that goes into selecting and transforming the variables into meaningful forms before building the neural network or deep learning algorithm. Without a framework of understanding, a lot of EHR data is simply a data dump that lacks clinical knowledge or visualization to provide appropriate scaffolding. You do need ingenuity, and you do need the right data. There are so many problems and complexities with data that innovation and ingenuity is lagging behind with healthIT.
The question is – is the answer you are looking for in the input data? If you have the answer in the data, you will be able to provide insights based on it. Innovation in healthcare predictions and patient records will come from looking at data sets that are actually predictive of health.
Dr. Rothman’s work in healthcare started with a medical error. His mother had valve replacement surgery and came through in good shape. Although initially she was recovering quickly, she started to deteriorate after a few days. And the problem was that the system made it difficult to see. Each day she was evaluated. Each day her condition was viewed as reasonable given her surgery and age. What they couldn’t see was that each day she was getting worse. They couldn’t see the trend. She was discharged and returned to the ED 4-days later and died.
As a scientist, he recognized that the hospital staff didn’t have everything they needed to avoid an error like this. He approached the hospital CEO and asked for permission to help them solve the problem. Dr. Rothman explained, I didn’t feel that the doctors had given poor medical care, this was a failure of the system.
The hospital CEO did something remarkable. They shared their data. In a safe system they allowed an expert in data science to come in to see what he could find in their patient records, rather than telling him he probably wouldn’t understand the printout. The hospital was an early adopter of EHR records, so they were able to look at a long history of data to find what was being missed. Using vital signs, lab tests, and importantly, an overlooked source of data, nursing notes, Dr. Rothman (and his brother) found a way to synthesize a unified score, a single number which captures the overall condition of the patient, a single number which was fed from the EMR and WOULD show a trend. There is an answer if you include the right data.
Doctors and nurses look at a myriad of data and synthesize it, to reach an understanding. Judy is right that a layman looking at random pieces of data will not likely gain much understanding, BUT they may. And with more help they might. Certainly, they deserve a chance to look. And certainly, the EMR and EHR companies have an obligation to present the data in some readable form.
Patients should be demanding data, they should be demanding hospitals give them usable care and normalize data based on their personal history to help save their lives.
Based on this experience, Michael and Steven built the Rothman Index, a measure of patient health based on analytics that visualizes data found in EHRs. They went on to found PeraHealth, which enables nursing kiosks to show the line and screens to see if any patients decline. In some health systems, an attending physician can get an alert about patients in danger. The visualization from the record isn’t just a screen by the patient, it is also on the physicians and nurses’ screens and includes warnings. Providers have time to evaluate what is wrong before it is too late. The data in the health record is made visual and can be a tool for providers.

Visualization of Patient Status with the Rothman Index and Perahealth
Is Perahealth everywhere? Not yet. For every innovation and potential improvement there is a period of time where slow adopters wait and invest in sure bets. Just like interoperable data isn’t an actuality in a system that desperately needs it, this is a basic step toward improving patient outcomes. Scaling implementation of an effective data tool is not always clear to hospital CMIO and CEO teams. The triage of what healthIT solution a healthcare system chooses to implement is complex. Change also requires strong collaborative efforts and clear expectations. Often, even if hospital systems know something provides benefits to patients, they don’t have the correct format to implement the solution. They need a strategy for adoption and a strong motivation. It seems that the strongest motivations are financial and outcomes based. The largest profit savings with the minimum effort usually takes adoption precedent. This should also be aligned with end users- if a nurse uses the system it needs to improve their workflow, not just give them another task.
One of the hospitals that is successfully collaborating to make patient data more useful and visual is Houston Methodist. I spoke to Katherine Walsh, Chief Nursing Officer from Houston Methodist about their journey to use EHR data with Perahealth. She explained it to me- Data is the tool, without great doctors and nurses knowing the danger zone, it doesn’t help. This reminded me of Faulkner’s reaction that not all patient data is useful. Clinical support should be designed around visible data to give better care. Without a plan, data is not actionable. Katherine explained that when nurses could see that the data was useful, they also had to make sure their workflow included timely records. When EHR data is actually being used in the care of patients, suddenly data entry workflow changes. When nurses and doctors can see that their actions are saving lives, they are motivated.

The process to change their workflow and visualize patient data did not happen overnight. In the story of Houston Methodist’s adoption of Perahealth, Walsh said they wanted to make sure they helped doctors and nurses understand what the data meant. “We put large screens on all the units- you can immediately see the patients that are at risk- it’s aggregated by the highest risk factor.” If you are waiting for someone to pull this data up on their desktop, you are waiting for them to search something. But putting it on the unit where you can see it makes it much easier to round, and makes it much easier to get a sense of what is going on. You can always identify what and who is at risk because it’s on a TV screen. The Houston Methodist team showed great leadership in nursing informatics, improving outcomes and using an internal strategy for implementation.
They normalize the variants for each person- a heart rate of 40 for a runner might be normal- then on the next shift 60 seems normal- then at 80 it also seems normal- you can tell them when you want an alert. To help with motivation, Walsh needed to make the impact of PeraHealth visual. They hung 23 hospital gowns around a room, representing the patients they had saved using the system.
The future of electronic health records will be about creating usable data, not just a data dump of fields. It is transforming EHRs from a cost hemorrhage to a life-saving tool through partnerships. Physicians don’t want another administrative task or another impersonal device. Nurses don’t want to go through meaningless measures and lose track of patients during shift changes. Show them the success they’ve had and let the data help them give great care.
Hospital administrators don’t want another data tool that doesn’t improve patient outcomes but has raised capital on vaporware. Creators don’t want more EHR companies that don’t know how to work with agile partners to create innovation.
The real ingenuity is in understanding – what data do you need? What data do patients need? Who can electronic healthcare record companies partner with to bridge the data divide?
We can bridge the gap of electronic health records that aren’t legible or useful to patients and create tools to save lives. Tools like those from PeraHealth are the result of a collaborative effort to take the data we have and synthesize it and visualize it and let care providers SEE their patients. This saves lives.
Without this, the data is there, it’s just not usable.
Don’t just give the patients their data, show them their health.
Article link: http://www.hospitalemrandehr.com/2017/10/13/visible-and-useful-patient-data-in-an-era-of-interoperability-failure/