Transforming Care focuses on new models of care, payment approaches, and patient engagement strategies that have the potential to reshape our delivery system to better meet the needs of the nation’s sickest and most vulnerable patients.
March 29, 2018 Issue
In Focus: Increasing Collaboration Among Physicians, Hospitals, and Postacute Providers to Reduce Variation and Spending
While many U.S. hospitals have concentrated on improving care transitions from hospital to home, far fewer have focused on the transition from hospitals to postacute care settings, including skilled nursing facilities. Increased awareness of variations in spending on postacute care and avoidable complications after hospital discharge — together with value-based payment arrangements — have prompted some physician groups, health systems, health plans, and postacute care providers to collaborate. Among their methods: assessing patients’ risk and identifying the most appropriate setting for them to recover and offering education to help patients regain their functionality and stay well. Better data about what works best for different patients and more aligned financial incentives among acute and postacute care providers could further these efforts.
By Martha Hostetter and Sarah Klein
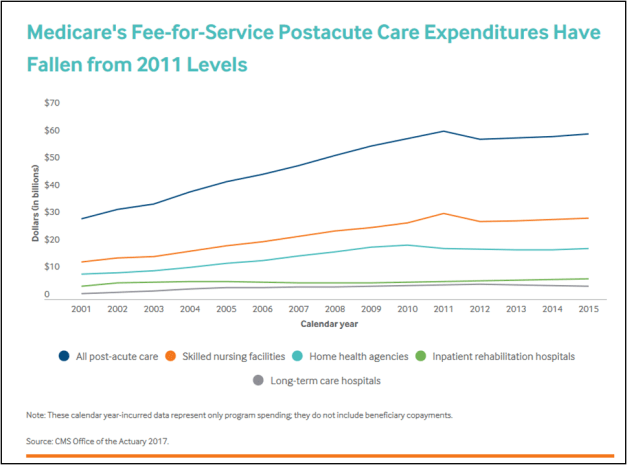
The Institute of Medicine’s 2013 study of Medicare spending upended a common assumption about the biggest drivers of regional variation: it was not hospital use that accounted for the largest the differences in spending across regions, but what happened after patients emerged from hospitals and began making use of skilled nursing facilities (SNFs) and home health care. The report also traced the dramatic rise in spending on SNF use and other types of postacute care, which more than doubled from 2001 to 2011, making it the fastest-growing sector of health care.1
The rise in the use of postacute care can be traced to Medicare’s decision in the 1980s to stop paying hospitals on a fee-for-service basis and instead make payments based on patients’ diagnoses, not how long they stay. This, together with the increased prevalence of capitated payments under managed care in the 1990s, led hospitals to reduce lengths of stay. Both factors fueled demand for postacute care providers — which include skilled nursing facilities (SNFs), home health agencies, inpatient and outpatient rehab facilities, and long-term hospitals — to help patients recover after surgery or acute illness and return home.2 Demand for postacute care also increased as a function of the aging of the U.S. population and the increasing prevalence of chronic and disabling conditions, which complicate recovery.3 About two of five Medicare beneficiaries end up needing some form of postacute care after a hospitalization.4
Read article: http://www.commonwealthfund.org/publications/newsletters/transforming-care/2018/march/in-focus